Fighting drug-resistant infections
Sep 6, 2011
Sep 6, 2011
A breakthrough in the fight against drug-resistant infections is one step closer following the discovery of the structure of NDM-1: a vicious form of bacteria that is currently resistant to the most powerful antibiotics available. The structure was determined by crystallography carried out at Diamond Light Source.
Medical Research Council (MRC) scientists at the Research Complex at Harwell (RCaH) in Oxfordshire, led by director Professor Simon Phillips, have produced a model of NDM-1 that will now enable researchers and pharmaceutical companies to progress towards potential new treatments. The research was published this week in the online journal Acta Crystallographica Section F: Structural Biology and Crystallization Communications.
 In recent years there has been growing concern that the usefulness of antibiotics could be coming to an end as the bacteria that cause disease become increasingly resistant to these drugs. Annually, over 25,000 people in the EU die of bacterial infections that have been able to outsmart even the newest antibiotics. The challenge to find new drugs that can overcome these superbugs is urgent and ongoing.
In recent years there has been growing concern that the usefulness of antibiotics could be coming to an end as the bacteria that cause disease become increasingly resistant to these drugs. Annually, over 25,000 people in the EU die of bacterial infections that have been able to outsmart even the newest antibiotics. The challenge to find new drugs that can overcome these superbugs is urgent and ongoing.
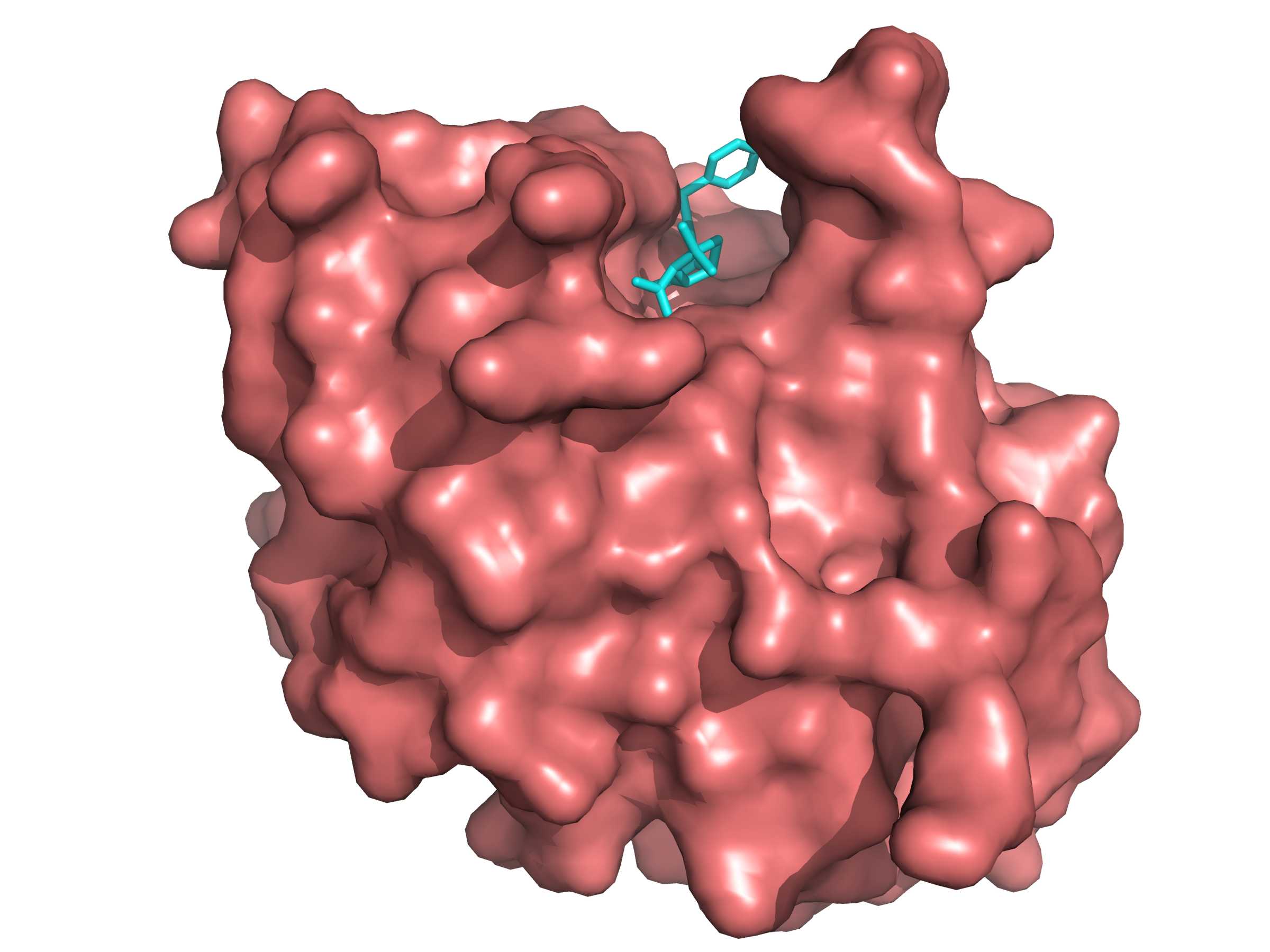
NDM-1 with Ampicillin pictured to the right.
The name NDM-1 relates to a particular enzyme carried by the resistant bacteria, called New Delhi Metallobetalactamase-1. This enzyme has the ability to break-up or ‘hydrolyse’ an antibiotic and make it ineffective.
Diamond Light Source is the UK's national synchrotron science facility, located at the Harwell Science and Innovation Campus in Oxfordshire.
Diamond Light Source Ltd
Diamond House
Harwell Science & Innovation Campus
Didcot
Oxfordshire
OX11 0DE
Copyright © Diamond Light Source. Diamond Light Source® and the Diamond logo are registered trademarks of Diamond Light Source Ltd
Registered in England and Wales at Diamond House, Harwell Science and Innovation Campus, Didcot, Oxfordshire, OX11 0DE, United Kingdom. Company number: 4375679. VAT number: 287 461 957. Economic Operators Registration and Identification (EORI) number: GB287461957003.