Mostly harmless
Polio is a neuromuscular disease which can cause paralysis and, in some cases, death. Following a series of epidemic outbreaks in the 20th century, a coordinated international effort to eradicate the disease was launched in 1988. Two highly effective vaccines have been central in the fight against polio: an inactivated form of the virus delivered by injection and a weakened form of the virus delivered orally. The oral vaccine has generally been preferred since it is significantly cheaper, easier to administer, and more effective at preventing the spread of the disease. However, the oral form is unstable at room temperature, necessitating cold storage during transport, which can prove challenging in remote or unstable regions where the disease remains endemic. A more serious drawback is the possibility of mutations, which cause the weakened virus to revert to a virulent form, leading to a polio outbreak.
.2020-02-21-13-40-40.jpg)
Many of these problems could be overcome by using virus-like particles (VLPs) as a vaccine. By mimicking the outer surface of a virus, which is recognised by our immune system, VLPs evoke an immune response; however, they are unable to replicate since they lack any genetic material, making them safe to use.
The coat of the poliovirus is an icosahedron built from four proteins, which are produced from a single protein through a series of processing steps. However, in the absence of viral genetic material, the final processing step does not occur; as a result, the partially processed proteins form an altered coat, which is not recognised by our immune system. To produce an effective virus from VLPs, the research team therefore used genes from a mutated poliovirus, which has more stable coat proteins that can form the correct shape even in the absence of genetic material.
Plant factories
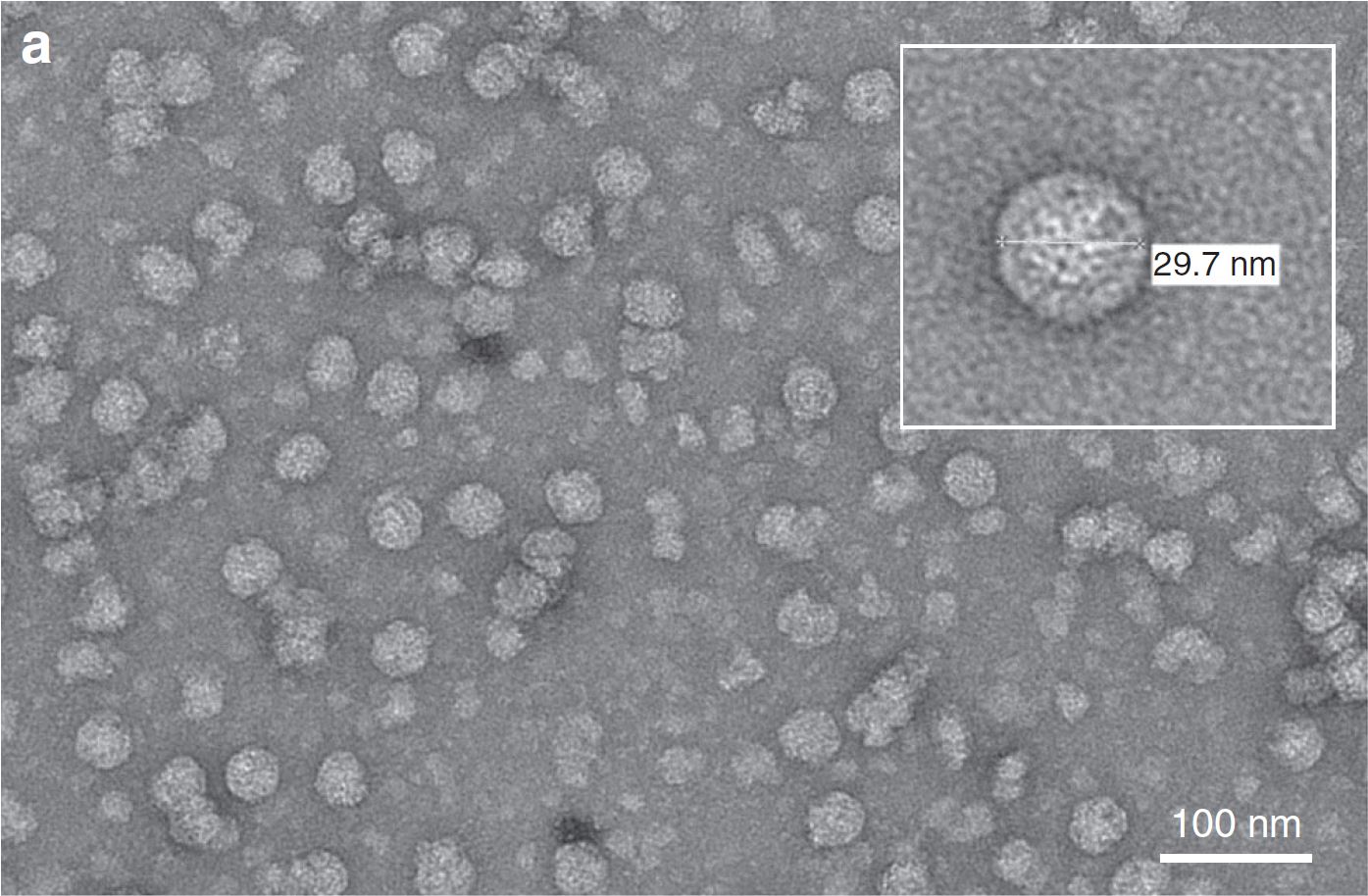
The team, led by Professor George Lomonossoff at the John Innes Centre, introduced the coat protein genes into the leaves of tobacco plants. Six days later, they harvested the leaves and extracted the polio VLPs. Transmission electron microscopy confirmed that the plant-produced VLPs made from the mutated coat protein gene were regularly shaped and of the correct size, while those made from the normal gene were irregularly shaped, as expected.
Next, the team turned to cryo-electron microscopy using the Titan Krios microscope and a direct electron detector at eBIC to get a clear look at the structure of the VLPs. Their analysis showed that the external features of the particles were identical to those of the poliovirus, including a key binding pocket on the surface. In other words, the tobacco plants had produced VLPs that look and feel identical to the poliovirus but lack its infectious qualities.
Finally, the team tested the efficacy of the VLPs as a vaccine. Mice engineered to carry the human receptor for poliovirus are susceptible to the disease, but treating these mice with the plant-produced VLPs protected them against polio infection as effectively as a regular polio vaccine. Unlike regular vaccines, the VLPs cannot revert to an infectious form, since they lack any genetic material, and they are also stable at room temperature.
In addition, because this approach requires only a single gene from the virus, production does not rely on maintaining stocks of live poliovirus, which could be accidentally released. The researchers also claim that plant-based VLP production is quicker than the traditional approach, potentially reducing the time needed to produce a vaccine from 10 months to 2-3 months.
.2020-02-21-13-40-41.png)
Despite the promising results, this study remains a proof-of-concept demonstrating that the technique works and that it may be a viable approach for tackling other viruses. “We don’t want to stop at a nice little lab technique. The next step is to scale up the production of the virus-like particles and to start human trials,” expands Prof Lomonossoff. If these trials are successful, a new vaccine, which avoids the shortcomings of the existing vaccines, could help to finally eradicate polio.
To find out more about the Titan Krios and eBIC, or to discuss potential applications, please contact Dr Alistair Siebert or Dr Daniel Clare: [email protected], [email protected]
Marsian J et al. Plant-made polio 3 stabilized VLPs – a candidate synthetic polio vaccine. Nature Communications (2017). DOI:10.1038/s41467-017-00090-w
Diamond Light Source is the UK's national synchrotron science facility, located at the Harwell Science and Innovation Campus in Oxfordshire.
Copyright © 2022 Diamond Light Source
Diamond Light Source Ltd
Diamond House
Harwell Science & Innovation Campus
Didcot
Oxfordshire
OX11 0DE
Diamond Light Source® and the Diamond logo are registered trademarks of Diamond Light Source Ltd
Registered in England and Wales at Diamond House, Harwell Science and Innovation Campus, Didcot, Oxfordshire, OX11 0DE, United Kingdom. Company number: 4375679. VAT number: 287 461 957. Economic Operators Registration and Identification (EORI) number: GB287461957003.